“I can feel like I’m going over a bump in the road or the top of a roller coaster.
I can also giggle, move my arms about or walk off. I’m not aware of doing this.”
Focal seizures are a type of seizure that start on one side of the brain. They are a common type of seizure. About 6 in 10 people with epilepsy have focal seizures. Some people with epilepsy only have focal seizures. Others will have different types of seizure too.
Focal seizures have different names. The name depends on whether you are able to respond well during the seizure, and remember what happened.
A focal seizure with preserved consciousness is when you can remember what happens during the seizure. You can also respond well to people and things around you.
This type of seizure used to be called a focal aware seizure, or a simple partial seizure.
“[I have] tingling in my face and hands, feeling like going up a big rollercoaster then coming down, feeling clammy and then muscle jerks and spasms on my left hand side. I am aware during my seizures then afterwards I struggle to speak and I am confused and extremely fatigued.”
A focal impaired consciousness seizure is when you cannot remember what happened during all of the seizure. Or, you cannot react appropriately, or with your usual speed. For example, you may not respond to a spoken instruction given to you by a family member in your usual way.
This type of seizure used to be called a focal impaired awareness seizure, or a complex partial seizure.
“I have focal impaired awareness seizures and, as I live alone, I don’t always immediately know that I’ve had one. Often, it will be the case that I become extremely fatigued and have an ‘unexplained’ headache.”

Some focal seizure symptoms can be noticed by other people. Healthcare professionals call these visible signs ‘observable manifestations’.
These can include:
Some focal seizure symptoms can’t be seen by others. Healthcare professionals call these focal seizures ‘without observable manifestations’.
These can include things like:

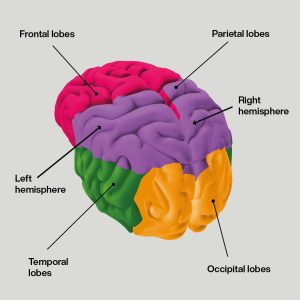
Focal seizure symptoms can be different for everybody. What you experience can depend on which area (lobe) of the brain is affected. It also depends on whether the seizure spreads to affect other areas of the brain. Some people experience one symptom during a focal seizure, while others have several.
‘Temporal’ sounds like this: tem-per-uhl or tem-pruhl
Focal seizures most commonly start in the temporal lobes. The temporal lobes are responsible for things like memory, hearing and understanding language.
Seizures starting in the temporal lobes are usually focal impaired consciousness seizures. You might remember what happens at the beginning and respond normally at first, but as the seizure continues, you may no longer be able to do so.
Here are some symptoms that might happen during a temporal lobe focal seizure:
You may feel confused or find it hard to speak for a short time after a temporal lobe seizure.
The frontal lobes in the brain are the largest lobes.
They are responsible for things like:
Some people who have frontal lobe seizures only have them in their sleep. They are sometimes mistaken for ‘parasomnias‘. These are sleep disorders where you have unusual behaviour or experiences during your sleep.
Frontal lobe seizures can also be mistaken for non-epileptic seizures (dissociative seizures).
Frontal lobe focal seizures don’t usually last long. They can often happen in clusters with several happening in a short space of time. Your level of consciousness may or may not be affected.
Here are some symptoms that might happen during a frontal lobe focal seizure:
‘Occipital’ sounds like this: ok-sip-i-tl
The occipital lobes are responsible for processing what we see (visual information).
Seizures starting in the occipital lobe often spread to involve other lobes. Here are some symptoms that can happen during an occipital lobe focal seizure:
‘Parietal’ sounds like this: puh-RIGH-uh-tuhl
The parietal lobes help us to understand things like:
Seizures starting in the parietal lobes often spread to involve other lobes. Here are some things that might happen during a parietal lobe focal seizure:
Some people with epilepsy use the word ‘aura’ to describe a particular feeling or symptom they have before the main onset of their seizure. For example, they may have:
An aura is actually a type of focal seizure that begins in just one part of the brain.
“I have focal impaired awareness seizures. I have a déjà vu aura that lasts up to around 5 seconds tops which gives me time to make sure everything is out of my hands.”
Sometimes a focal seizure can spread to both sides of the brain, leading to a generalised seizure. When this happens it is called a focal to bilateral tonic-clonic seizure. Some people call the focal seizure that comes before a generalised seizure an aura.
Most focal seizures are short, usually lasting between a few seconds and a few minutes. But they can be shorter or longer for some people.
One study found that focal seizures with preserved consciousness generally tended to last between 1 second and 3 minutes. The average duration was around 27 seconds.
Focal seizures with impaired consciousness tended to be a little longer. These seizures typically lasted between 10 seconds and 4 ½ minutes, with an average of 43 seconds.
Some people feel fine straight after a focal seizure, while others need time to recover. You might be able to get back to what you were doing straight away. Or you might feel confused or tired for some time afterwards.
This is sometimes called the ‘post-ictal phase’. Some people might need to sleep during this phase. Other people might wander without being aware. This can be more likely with temporal lobe seizures, but it can happen with other types of focal seizure too. It is important to stay with someone if they wander after a seizure, to help guide them from danger.
Some people find they have temporary weakness or can’t move part of their body after they’ve had a seizure. This is called Todd’s paralysis (or Todd’s paresis). It can last from a few minutes up to 36 hours, before going away. Todd’s paralysis is not the same as weakness or difficulty moving caused by an injury during a seizure.
Try to learn as much as possible about your seizures. This includes if anything is likely to trigger them, and what can help you if you have one.
Many people search for information after a first focal seizure. If you think you have had a focal seizure, here’s what you can do:
Find more information on our diagnosis page.
Someone having a focal seizure may, or may not, be aware of what is happening. Focal seizures can be frightening and disorientating for the person having the seizure. Being kind, calm and reassuring can really help.
“The best thing is for people to stay with me and make sure I’m safe. It’s horrible coming around and being confused about where I am or not remembering how I’ve hurt myself.”
Try to avoid doing anything that might frighten the person having a seizure. Don’t make any sudden movements, shake them, or shout. Even if the person is aware, they could feel confused and unsteady for a while after the seizure. They may feel tired, and need time to rest and recover.

Take a look at our quick tips for focal seizure first aid below.
It’s important that you don’t hold the person down or move them unless they are in danger. You shouldn’t try to bring them round and never give them anything to eat or drink until they recover.
Call for an ambulance if:
Sometimes a focal seizure can progress into another type of seizure, such as a tonic-clonic seizure. Find out more about tonic-clonic first aid.
We have more information about other seizure types and how to help someone from our main first aid page.
There are at least 21 types of epileptic seizures, each with its own name. The International League Against Epilepsy is the main organisation for epilepsy healthcare professionals. It recommends naming seizures as accurately as possible so people get the right support and treatment.
As we learn more about seizures, their names have changed over time. You may also have your own names for your seizures. You can use whatever name you are comfortable with for your seizure type.
The International League Against Epilepsy published the latest seizure classification in 2025. Read the paper for free.
The main treatment for epilepsy is taking epilepsy medicines. They don’t cure epilepsy, but they can help to prevent focal seizures from happening. Find out more about epilepsy medicines.
If you have epilepsy, the law can protect you from disability discrimination in certain circumstances. This is true whether you feel that you have a disability or not. Find out more here.
If your seizures affect your ability to do day-to-day activities, you may be eligible for certain disability benefits. Find out more here.
There are different rules for driving with epilepsy. These rules depend on the type of seizures you have, when they happen and what type of vehicle you want to drive.
If you have seizures that affect your consciousness, you must be seizure free for at least 12 months, before you’re allowed to drive.
If your seizures never affect your consciousness, the DVLA may allow you to drive without being seizure free. This is only if you meet certain conditions. Find out more on our driving rules page or speak to our helpline on 0808 800 5050.
Some people with epilepsy use the word aura to describe symptoms that come before a full seizure. These symptoms are sometimes a focal seizure starting on one side of the brain. This can then spread to both sides of the brain and turn into a different type of seizure.
We can help you adjust to living with focal seizures. Call our helpline on 0808 8005050 to ask about the support that we offer.
Our expert advisors can help you with any questions you might have about focal seizures or anything else related to living with epilepsy.
This page is printable and can be downloaded. We also have accessibility tools available at the top of the page. These tools can also translate this page into different languages.
Thank you to our expert reviewers and health information volunteers, for contributing to and reviewing this content. Thank you also to everyone who shared their experiences for the quotes used on this page.
Find out more about how you can help us create our health information.
Ioannou P, et al., (2022), The burden of epilepsy and unmet need in people with focal seizures. Brain Behav. 2022;12(9):e2589. doi: 10.1002/brb3.2589. Epub 2022 Aug 26. PMID: 36017757; PMCID: PMC9480957.
Gupta, S. et al., (2017), Understanding the burden of focal epilepsy as a function of seizure frequency in the United States, Europe, and Brazil. Epilepsia Open, 2: pp. 199-213. Available at: https://doi.org/10.1002/epi4.12050
Beniczky S, et al., (2025), Updated classification of epileptic seizures: Position paper of the International League Against Epilepsy. Epilepsia. 2025; 66: 1804–1823. Available at: https://doi.org/10.1111/epi.18338
McIntosh et al., (2023) StatPearls Temporal Seziure, Available at: https://www.ncbi.nlm.nih.gov/books/NBK549852/ (Accessed: 13 August 2025)
Patel et al., (2023), StatPearls, Neuroanatomy, Temporal Lobe. Available at : https://www.ncbi.nlm.nih.gov/books/NBK519512/ (Accessed: 12 August 2025)
International League Against Epilepsy (2024), Temporal Lobe Seizure, Available at: https://www.epilepsydiagnosis.org/seizure/temporal-overview.html, (Accessed: 12 August 2025)
International League Against Epilepsy (2024) Frontal lobe seizure. Available at https://www.epilepsydiagnosis.org/seizure/frontal-lobe-overview.html (Accessed: 12 August 2025).
Jawabri et al., (2023), StatPearls, Physiology, Cerebral Cortex Functions. Available at : https://www.ncbi.nlm.nih.gov/books/NBK538496/ (Accessed: 12 August 2025)
International League Against Epilepsy (2024) Occipital lobe seizure. Available at https://www.epilepsydiagnosis.org/seizure/occipital-overview.html (Accessed: 12 August 2025)
International League Against Epilepsy (2024) Parietal lobe seizure. Available at https://www.epilepsydiagnosis.org/seizure/parietal-overview.html (Accessed: 12 August 2025)
Blom JD. (2016) Alice in Wonderland syndrome: A systematic review. Neurol Clin Pract. 6(3), pp. 259-270. Available at: https://www.neurology.org/doi/10.1212/CPJ.0000000000000251
Ighodaro ET., et al., (2023), StatPearls Focal Onset Seizure, Available at: https://www.ncbi.nlm.nih.gov/books/NBK500005/, (Accessed: 13 August 2025)
Larsen, PG, et al., (2022), Duration of epileptic seizure types: A data-driven approach. Epilepsia, Vol 64 (2), pp: 469-478, Available at: https://onlinelibrary.wiley.com/doi/full/10.1111/epi.17492
Xu SY, et al., (2020), Frequency and Pathophysiology of Post-Seizure Todd’s Paralysis. Med Sci Monit. 5;26:e920751. Available at: https://medscimonit.com/abstract/index/idArt/920751