Jump straight to the information you need
What is the ketogenic diet?
The ketogenic diet is a specialist medical diet that is high in fat with restricted carbohydrates. Sometimes you might see it called the ‘keto diet’.
There are different types of ketogenic diets and a specialist dietitian will support you to decide which one is best for you.
They will make sure the diet is safe and meets your nutritional needs.
The ketogenic diet talks about food in terms of fats, carbohydrates and proteins. It is important to remember that this diet is a specialist treatment for some people with epilepsy.
-
What is a fat?
Fat is a source of energy. When your body digests fatty foods, such as oils and animal fats, it produces fatty acids.
When these are broken down in the liver, they produce ketone bodies. Ketone bodies can be used by the body as an energy source.
-
What is a carbohydrate?
Carbohydrates are in foods such as bread, pasta and potatoes, as well as fruits and vegetables. They are made up of sugars, starches, and fibre.
The body turns these sugars into glucose which is then used as energy.
- What is protein?
-
Finding recipes
Meals that follow the ketogenic diet can be tasty too. Matthew’s Friends has recipes and a cooking channel on YouTube.
There are also recipe books written by specialists, such as Ketocooking: A Practical Guide to the Ketogenic Diet, by Judy Nation, J. Helen Cross, Ingrid E. Scheffer.
Who might benefit from a ketogenic diet?
The ketogenic diet is a treatment option for some people whose seizures are hard to control with anti-seizure medication.
The National Institute for Health and Care Excellence (NICE) guidance for treatment of epilepsy says that the ketogenic diet can be considered for:
- People whose seizures can’t be stopped with epilepsy medicine. They may have tried other treatments which have also not worked or are not appropriate.
- People with certain epilepsy syndromes.
If you think the ketogenic diet might help you or your child, you should discuss this with an epilepsy specialist.
-
Ketogenic diet in children
Some high quality studies have shown that children can have a good response to the ketogenic diet and some will become seizure free.
One study found that children given ketogenic diets may be up to three times more likely to achieve seizure freedom and up to six times more likely to experience a 50% or greater reduction in seizures.
There have also been studies that show the benefits in children under the age of two, but there haven’t been many studies involving this age group.
Children who are not yet on solid food can still benefit from the ketogenic diet. It is possible to be prescribed a formula-based diet. This can also be used in children and adults with feeding tubes.
Children can face peer pressure about food. Not having the same freedom as others around food may have an impact on their mental health.
It is important to talk to your child about treatment so they can understand why they must eat in a certain way.
-
Ketogenic diet in adults
Many adults report that the ketogenic diet has helped them but more evidence is needed to assess how well it works in adults.
There are studies that show it reduces seizures in adults, but more evidence is needed to balance the benefits and the risks.
No good quality studies have shown that the ketogenic diet can lead to seizure freedom for adults, however, adults given the ketogenic diets may be up to five times more likely to have fewer seizures.
The ketogenic diet does not work for everyone, and it is not possible to say who it will help.
For many adults, the ketogenic diet is effective, but some of the difficulties people report include:
- Not having enough information – a epilepsy specialist or charity such as Matthew’s Friends can offer support with this
- It can be more expensive, and take more effort to keep up with a special diet
- If you work, and are out of the house a lot, the restrictions might not be practical for your lifestyle. But alternatives to the classical ketogenic diet such as the Modified Atkins Diet (MAD) allow for more flexible food choices when dining out
Even as an adult, it is still important to be under medical supervision for these diets.
It will need to be prescribed by a specialist who can also think about any other health conditions you have or medicines that you take.
How does the ketogenic diet work?
The ketogenic diet has been used to treat epileptic seizures since the 1920s but how it works is still not completely known. There are many theories about how the ketogenic diet affects the brain.
One theory is that having more ketones in the brain might help prevent seizures. Our bodies can use two types of energy: a sugar (glucose) that comes from carbohydrate foods, or ‘ketones’ that come from the fats we eat. During the ketogenic diet, the body produces more ketones, which are used as fuel and less glucose is used.
Making ketones gives your brain and body an alternative type of energy to use.
Matthews Friends have produced a simple animated video for children that explains more about using the ketogenic diet as an epilepsy treatment.
Why do you need medical supervision to go on this diet?
A team of epilepsy specialists who are experts in the diet should manage ketogenic diet therapy. This is because it is a restrictive diet and close monitoring is needed particularly in growing children.
The ketogenic diet needs to be carefully worked out for each person. You will also need advice on taking vitamins and other special supplements.
People can have a very individual response to the ketogenic diet. Some people will have unwanted side effects, especially at first.
These might include weight loss, constipation or diarrhoea and high cholesterol. Your ketogenic diet team should be able to help you manage most of these but some people still find the side effects difficult to cope with.
If you have certain other medical conditions, it may mean that the ketogenic diet is not safe for you to follow. There are some metabolic disorders that would make the ketogenic diet unsuitable.
Some of these are conditions where the body cannot break down fats into energy normally.
Starting a strict diet can be challenging, especially as a family. It can be helpful to talk it through with your specialist team and make decisions together.
In order for the ketogenic diet to work, the amount of protein, carbohydrate and fat are prescribed by a dietitian, which means that some or all of your foods may need to be weighed and measured.
Do I need to take epilepsy medicine as well?
Many people use a ketogenic diet alongside other treatments such as anti-seizure medicines or vagus nerve stimulation. More research is needed to understand how different medicines might interact with the ketogenic diet.
There are some studies that suggest the diet and certain epilepsy medicines might be less effective when used together, but more and better evidence is needed before we can say this for certain. This is why medical supervision is needed so that you can make informed decisions about these complicated issues.
Nearly 9 out of 10 children on the ketogenic diet still also take at least one anti-seizure medicine. But many are able to reduce the amount of medicine over time, which can help with some side effects.
Types of ketogenic diets
There are different versions of the ketogenic diet.
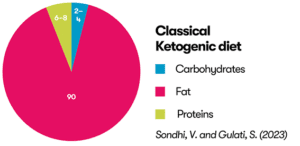
The classical ketogenic diet is the most restrictive type of diet where carbohydrates, proteins and fats are all measured.
- MAD/MKD diet
- MCT diet
-
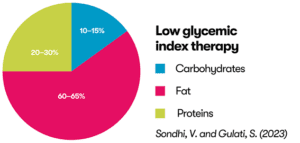
LGIT diet
The low glycaemic index treatment (LGIT) is another related diet. Carbohydrates are restricted and fat is encouraged.
Evidence for the effectiveness of this diet is limited.
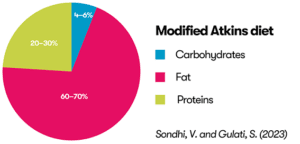
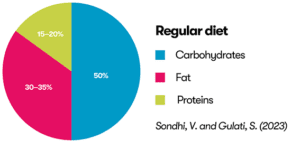
You can see the differences between the ketogenic diets in the diagram below.
These modified diets are less strict than the classical ketogenic diet and you may not need to weigh all your food. The MAD/ MKD is becoming more popular for children because it’s less restricted but still has a good outcome.
Matthew’s Friends
This charity is all about medical ketogenic dietary therapies. It provides a huge amount of information, training, research and support for medical professionals, families and patients. This includes their website, YouTube tutorials and cooking channels and social media.
Matthew’s Friends has online ketogenic support forums for families on Facebook. They also provide professional training including webinars and eLearning.
Their main website has detailed information on the various ketogenic diets for children and adults and a list of NHS and private ketogenic diet centres in the UK and contact details of specialists.
The Daisy Garland charity
The Daisy Garland charity offers information about childhood epilepsy. It specialises in the ketogenic diet and the Modified Atkins diet. It helps fund dietitians in the NHS around the country.
-
Sources
D’Andrea Meira, I. et al. (2019) ‘Ketogenic Diet and Epilepsy: What We Know So Far’, Frontiers in Neuroscience, 13, p. 5. Available at: https://doi.org/10.3389/fnins.2019.00005.
Asp, N.-G. (1996) ‘Dietary carbohydrates: classification by chemistry and physiology’, Food Chemistry, 57(1), pp. 9–14. Available at: https://doi.org/10.1016/0308-8146(96)00055-6.
10 high protein foods | BBC Good Food (no date). Available at: https://www.bbcgoodfood.com/howto/guide/best-sources-protein (Accessed: 21 February 2024).
Nuttall, F.Q. and Gannon, M.C. (2013) ‘Dietary Protein and the Blood Glucose Concentration’, Diabetes, 62(5), pp. 1371–1372. Available at: https://doi.org/10.2337/db12-1829.
Nation, J., Cross, J.H. and Scheffer, I.E. (2013) Ketocooking: A Practical Guide to the Ketogenic Diet. 1st edn. The Homewood Press.
Overview | Epilepsies in children, young people and adults | Guidance | NICE (2022). NICE. Available at: https://www.nice.org.uk/guidance/ng217 (Accessed: 14 November 2023).
Neal, E.G. et al. (2008) ‘The ketogenic diet for the treatment of childhood epilepsy: a randomised controlled trial’, The Lancet Neurology, 7(6), pp. 500–506. Available at: https://doi.org/10.1016/S1474-4422(08)70092-9.
Schoeler, N.E. et al. (2023) ‘Classic ketogenic diet versus further antiseizure medicine in infants with drug-resistant epilepsy (KIWE): a UK, multicentre, open-label, randomised clinical trial’, The Lancet Neurology, 22(12), pp. 1113–1124. Available at: https://doi.org/10.1016/S1474-4422(23)00370-8.
Sharma, S. et al. (2013) ‘Use of the modified Atkins diet for treatment of refractory childhood epilepsy: A randomized controlled trial’, Epilepsia, 54(3), pp. 481–486. Available at: https://doi.org/10.1111/epi.12069.
Liu, H. et al. (2018) ‘Ketogenic diet for treatment of intractable epilepsy in adults: A meta-analysis of observational studies’, Epilepsia Open, 3(1), pp. 9–17. Available at: https://doi.org/10.1002/epi4.12098.
Lyons, L. et al. (2020) ‘Use of ketogenic diet therapy in infants with epilepsy: A systematic review and meta-analysis’, Epilepsia, 61(6), pp. 1261–1281. Available at: https://doi.org/10.1111/epi.16543.
Hosain, S.A., La Vega-Talbott, M. and Solomon, G.E. (2005) ‘Ketogenic diet in pediatric epilepsy patients with gastrostomy feeding’, Pediatric Neurology, 32(2), pp. 81–83. Available at: https://doi.org/10.1016/j.pediatrneurol.2004.09.006.
Erkent, I., Ilgaz, F. and Dericioglu, N. (2023) ‘Difficulties in the implementation of the ketogenic diet in adult patients with refractory epilepsy’, Epilepsy & Behavior, 144, p. 109234. Available at: https://doi.org/10.1016/j.yebeh.2023.109234.
Kossoff, E.H. et al. (2018) ‘Optimal clinical management of children receiving dietary therapies for epilepsy: Updated recommendations of the International Ketogenic Diet Study Group’, Epilepsia Open, 3(2), pp. 175–192. Available at: https://doi.org/10.1002/epi4.12225.
Martin-McGill, K.J. et al. (2020) ‘Ketogenic diets for drug‐resistant epilepsy’, Cochrane Database of Systematic Reviews [Preprint], (6). Available at: https://doi.org/10.1002/14651858.CD001903.pub5.
Armeno, M.L. and Kossoff, E.H. (2023) ‘Let food be thy medicine. The interaction between ketogenic diet therapy and anti-seizure medications: A systematic review’, Epileptic Disorders, 25(1), pp. 18–27. Available at: https://doi.org/10.1002/epd2.20055.
‘Modified Ketogenic Diets – MAD & LGIT’, Matthews Friends. Available at: https://www.matthewsfriends.org/keto-therapies/keto-introduction/modified-ketogenic-diets-mad-lgit/ (Accessed: 24 January 2024).
Cambridge University Hospitals (2022) The MCT diet – information for children and their carers Available at: https://www.cuh.nhs.uk/patient-information/the-mct-diet/ (Accessed: 14 November 2023).
Sondhi, V. and Gulati, S. (2023) ‘Low glycemic index therapy: What it is and how it compares to other epilepsy diets’, in Diet and Nutrition in Neurological Disorders. Elsevier, pp. 449–470. Available at: https://doi.org/10.1016/B978-0-323-89834-8.00047-7.
Got any questions?
Our expert advisors can help you with any questions you might have about the ketogenic diet or anything else related to living with epilepsy.







