What would you like to find out about today?
Who gets Sturge-Weber syndrome?
Sturge-Weber syndrome is rare. It’s thought to affect between 2 and 5 in 100,000 children.
The condition is something you’re born with and is caused by a change (called a ‘mutation’) in a gene, called GNAQ. This mutation develops in a growing baby before they’re born – it’s not something that’s passed from parents.
Everyone who gets Sturge-Weber syndrome is affected differently. There are lots of symptoms and they all vary from person to person. Sturge Weber UK is a charity that supports people affected by this syndrome and has lots of information and stories about personal experiences.
Symptoms of Sturge-Weber syndrome
Sturge-Weber syndrome has a number of different symptoms. More than three quarters of children have seizures, around half will develop glaucoma, and more than half will have learning difficulties and developmental delays.
Not every child will be affected by all of the symptoms; it often depends on how severe the brain damage is as to the level of problems they may face.
-
Birthmark
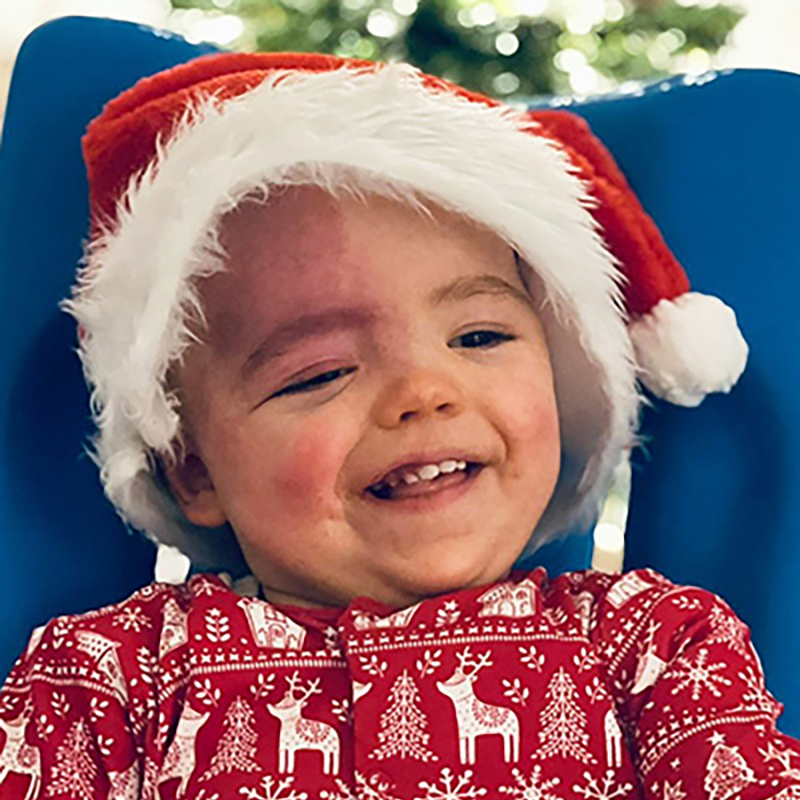
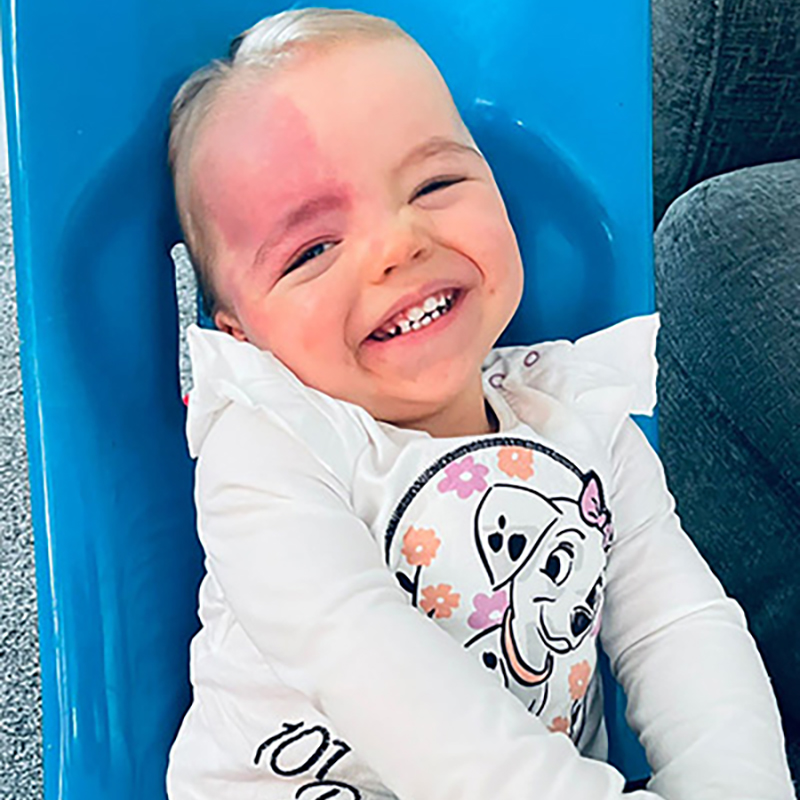
If your baby has Sturge-Weber syndrome, the first sign is usually the birthmark or ‘port wine stain’, which is normally noticeable straight after birth. The medical word for this is ‘angioma’. The birthmark:
- Is flat and appears as deep red or purple on white skin, or very dark patches on brown or black skin
- Occasionally it can be very pale, or not even visible at first, but it tends to become darker with age
- Usually covers the forehead and upper eyelid, but may extend down the cheek
- Usually just affects one side of the face, but rarely might affect both sides
- Rarely may involve other parts of the body, like the neck and arms
- Won’t grow any bigger as your child gets older
-
Seizures
At least three-quarters of children with Sturge-Weber syndrome will have seizures. These are caused by the growth of blood vessels on the surface of the brain. Seizures usually start before your baby is 1. They may include:
- Focal motor seizures – these cause repeated muscle jerks, called clonic seizures, in one area of your child’s body. They may spread to affect their whole body
- Atonic seizures – where your child becomes floppy and suddenly falls down
- Myoclonic seizures – these cause sudden jerking movements, usually on one side of the body
- Infantile epileptic spasms – where your baby’s body briefly stiffens on one side or both sides of their body
Seizures can happen often, and many times a day. They may also be prolonged, meaning that they last a long time. This may result in an emergency situation, called convulsive status epilepticus. Your child will need emergency treatment if they develop status. Your child’s specialist will discuss a care plan for you and your family to help you to prepare and manage situations like this.
Children with Sturge-Weber syndrome often develop a weakness in one side of their body after a seizure. This is known as hemiparesis or hemiplegia. This may be temporary at first, but can become worse and last for longer with repeated seizures.
Some children also have episodes of weakness without having seizures, which are similar to strokes in adults. Sometimes this weakness may be permanent. Your child may also develop migraine-like headaches as they get older.
-
Vision
Children with Sturge-Weber syndrome also often develop problems with sight or vision. They may lose vision on part or all of one side of their visual field. This will usually be the same side of their body as they get weaknesses. This is called ‘hemianopia’.
Around half of children develop a condition called glaucoma. This is raised pressure in the eye. It can cause loss of sight if it’s not treated. Children who have a birthmark involving their eyelid are more likely to be affected. Glaucoma can be present from birth, or it may develop later on during childhood.
-
Development and learning problems
Developmental delay, learning and behaviour problems affect more than half of children with Sturge-Weber syndrome. These problems can be mild or severe and may happen more often in children who have more frequent or severe seizures.
Diagnosing Sturge-Weber syndrome
If your baby is born with a ‘port-wine’ birthmark on the upper part of their face, they should be assessed for Sturge-Weber syndrome. They should see a specialist doctor called a paediatrician.
Your child will need to have a brain scan to diagnose Sturge-Weber syndrome. This will usually be an MRI (magnetic resonance imaging). The scan is usually done with a dye or ‘contrast’. This can show up parts of the brain affected by Sturge-Weber syndrome. Sometimes other types of scan may be used, such as a CT scan.
They will also have an EEG (electroencephalogram) to look at the electrical activity in their brain, and how this relates to their seizures.
Your child should also be referred to an eye specialist (ophthalmologist) to test for glaucoma. The paediatrician can also refer them to an expert in children’s epilepsy called a paediatric neurologist.
Treatment for Sturge-Weber syndrome
Treatment for Sturge-Weber syndrome is mainly aimed at trying to control the seizures. Reducing the number or severity of the seizures can help to prevent the other problems associated with the condition.
Epilepsy medicines
Your child’s doctor may suggest several different epilepsy medicines to control their seizures.
These may include:
- Carbamazepine
- Levetiracetam
- Lamotrigine
- Sodium valproate
- Topiramate
Sodium valproate can harm an unborn baby if taken during pregnancy. For this reason, if your child is able to get pregnant, or may do when they’re older, your child’s paediatrician will usually suggest an alternative medicine. If they do recommend treatment with sodium valproate, they will discuss the risks and benefits with you and your child first.
Your child’s specialist will discuss a ‘rescue’ or emergency care plan with you to treat any prolonged or repeated seizures.
Information about treatments for children can be found on the Medicines for Children website.
Surgery
Many children with Sturge-Weber syndrome find their epilepsy becomes resistant to medical treatment. If this happens, your child’s specialist may suggest considering epilepsy brain surgery. Surgery involves removing or disconnecting the part of the brain that causes the seizures. To be considered for surgery, your child will need to be referred to a specialist centre. This will be done through the ‘Children’s Epilepsy Surgery Service’ (CESS).
Treatment for other problems
Your children may see a range of different doctors and other health professionals to treat other problems related to their condition.
If they are experiencing stroke-like episodes, they may be offered daily low-dose aspirin. There are certain risks of taking aspirin in children, and your child’s paediatrician or paediatric neurologist will discuss this with you.
If glaucoma develops, it can be treated with daily eye drops and if necessary, an operation.
The birthmark can be managed by make-up or laser treatment.
Your child will need regular follow-up with a specialist eye doctor (ophthalmologist) and a skin specialist (dermatologist).
Outlook of Sturge-Weber syndrome
There is a varied outlook for children with Sturge-Weber syndrome. If your child’s seizures are well controlled, or less severe, there is often a much more positive outlook.
If both sides of your child’s brain are affected, this often means the seizures are worse, and any learning disabilities or visual problems are more severe. Unfortunately, if both sides of the brain are damaged, surgery is much less likely to help.
Sadly, Sturge-Weber syndrome tends to slowly get worse with age. To what level often depends on how well the seizures are controlled.
Problems such as seizures and stroke-like episodes can continue throughout life. If your child has learning disabilities this might affect their education, and may present challenges in the workplace or living independently. There is a lot of support available to help those with learning difficulties, as well as Sturge-Weber syndrome. We have listed some of these organisations at the bottom of this page.
Other names for Sturge-Weber syndrome
Sturge-Weber syndrome may also be called:
- Encephalofacial angiomatosis
- Encephalotrigeminal angiomatosis
The term ‘encephalo’ means it’s to do with the brain, while ‘facial’ or ‘trigeminal’ refers to the area where you get the birthmark. ‘Angiomatosis’ is the name for a growth of blood vessels. It’s this abnormal growth of blood vessels that causes the symptoms associated with Sturge-Weber syndrome.
Sturge-Weber syndrome is one of a group of conditions called ‘neurocutaneous syndromes’. This is because it affects the brain (‘neuro’) and also the skin (‘cutaneous’).
Support
Contact – for families with disabled children
Freephone helpline: 0808 808 3555
Email: helpline@contact.org.uk
Support and information for people with hemiplegia and their families in the UK.
Freephone helpline: 0808 808 1111
Email: helpline@mencap.org.uk
Sturge Weber UK
Support group for families and adults affected by Sturge Weber syndrome.
Email: support@sturgeweber.org.uk
Providing UK-based support for anyone with a birthmark and their families.
Email: info@birthmarksupportgroup.org.uk
Phone: 07825 855 888